|
12/7/2023 0 Comments Aetna timely filing limit 2016  
AdvancedHEALTHTimely-Filing-Grid2016 Created Date: 7:57:13 PM. She is responsible for creating, editing, and managing all content, design, and interaction on the company website and social media channels in order to promote CIPROMS as a thought leader in healthcare billing and management.įor more information about how we use your data, please review our privacy policy. INSURANCE CLAIM TYPE TIMELY FILING LIMITS Aetna Initial Claim 120 days from DOS. Charity Singleton CraigĬharity Singleton Craig is a freelance writer and editor who provides communications and marketing services for CIPROMS. For use or reprint in your blog, website, or publication, please contact us at. 
Below, I have shared the timely filing limit of all the major insurance Companies in United States. 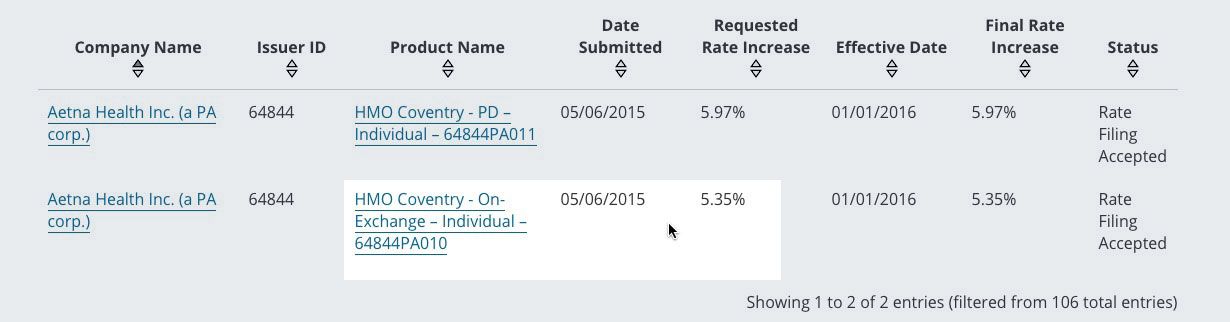
However, Medicare timely filing limit is 365 days. in favor of Aetna but limited the settlement portion to the 30,000 limit. The timely filing limit varies by insurance company and typically ranges from 90 to 180 days. Meanwhile Medicare’s filing limit remains 12 months from the date of service, and traditional Indiana Medicaid has a 180-day filing limit.įor more information about the change, review Anthem’s Provider Communications article “ Reminder: Changes to timely filing requirements coming in October.” 387 Aetna did not defend the action but instead settled the case for 35,000. Indiana’s Medicaid Managed Care Entities also have a 90-day filing limit. The new 90-day requirement reflects Anthem’s commitment to “simplify processes, improve efficiencies, and better support coordination of care.” The change also aligns Anthem with other commercial payers, including Aetna, Cigna, and United Healthcare, all of whom have 90-day timely filing limits for claims. Health Care Timely Filing Limits for all Insurances admin Timely filing limits for some of the important insurances like Aetna timely filing limit, Medicare timely filing, BCBS timely filing, UHC, Cigna timely filing limits and many more in the following table. Quantity limits For certain drugs, we limit the amount. “One hundred eighty days has been the Anthem Blue Cross and Blue Shield (Anthem) standard since 2007,” the payer explained. It means that Aetna Better Health of California agrees that the care is necessary for your health. In 2016, when some professional and ancillary provider contracts inadvertently included a 90-day filing limit, Anthem issued a blanket correction, confirming their 180-day filing limit at that time. Beginning October 1, 2019, all claims will be subject to a 90-day filing requirement, and according to the payer, “Anthem will refuse payment if submitted more than 90 days after the date of service.”įor years, Anthem’s timely filing limit has been 180 days. Learn more about our Medicare Advantage PPO plans. The insurance provider is supposed to, in a timely. Cigna timely filing (Commercial Plans) 90 Days for Participating Providers or 180 Days for Non Participating Providers. With Aetna Medicare Advantage PPO plans, you can visit any doctor in or out of our provider network who accepts Medicare and our plan terms. Follow the list and Avoid Tfl denial.Anthem is changing their timely filing limit for professional claims. When an injury or illness limits or prevents you from working, you will want to file for LTD benefits. One such important list is here, Below list is the common Tfl list updated 2022. There is a lot of insurance that follows different time frames for claim submission. One of the common and popular denials is passed the timely filing limit. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
